Two young adults, an 18-year-old and 21-year-old, recently died, and 18 others were hospitalized, in an outbreak of meningitis in Kent, England.
People in their teens and early 20s are considered to be at greater risk for this type of rare but serious bacterial infection called meningococcal group B that can lead to meningitis, an inflammation in the membranes that cover the spinal cord and brain. The outbreak seems to have occurred in people, including students from two universities, who attended a nightclub in early March.
More than 10 percent of those who get meningococcal disease will die of it, even with treatment, and survivors can be at risk of limb loss, kidney damage and nervous system issues, including hearing loss and brain damage. Prompt medical treatment can reduce the chances of developing these severe complications.
Thanks in large part to the success of meningococcal vaccines, these types of infections are uncommon in the United States, though cases have risen over the past few years. There were 503 confirmed and probable cases in the United States in 2024, the highest level since 2013.
“The hard part with this infection, and the reason the vaccines have been so important, is that [it] progresses in hours, not days,” said J. David Beckham, chief of the division of infectious diseases and geographic medicine at the University of Texas Southwestern Medical Center. “It’s considered one of the true medical emergencies in medicine.”
Here’s what to know about meningitis, including the symptoms to look out for, signs you need medical care ASAP, who’s most at risk and how to best protect yourself from getting infected in the first place.
Bacterial meningitis is the most concerning type
Somewhat confusingly, “people use meningitis as a blanket term,” said Katrine Wallace, an epidemiologist and adjunct assistant professor at the University of Illinois at Chicago’s School of Public Health. It broadly refers to swelling in the brain and spinal cord and can have many different causes, including viral, fungal and bacterial infections as well as parasites, cancer or certain drugs. Most often, meningitis is triggered by a viral or bacterial infection.
When you hear about meningitis outbreaks like the one in England, they usually are meningococcal meningitis, Wallace explained, which is a form of meningitis caused by a specific type of bacteria called Neisseria meningitidis. These bacteria can live in the back of the throat and spread through close contact with an infected person’s saliva.
There are different strains, or serogroups, that can cause infections in humans, including serotypes A, B, C, W, X and Y. Confirmed cases in the Kent outbreak have been found to be group B.
Physicians worry about bacterial meningitis more than other types, said Richard Martinello, an associate professor of medicine and pediatric infectious diseases at Yale School of Medicine. That’s because about 1 in 6 bacterial meningitis cases worldwide are fatal, according to the World Health Organization.
Meningococcal disease “can be very aggressive and move quickly,” said David Boulware, a professor in the division of infectious diseases and international medicine at the University of Minnesota. So it’s important to seek emergency care right away if you believe you or a loved one may have been exposed.
It’s easy to mistake the symptoms for less serious conditions
Meningitis can cause a range of possible symptoms, including some that could be mistaken for other illnesses, like a fever, headache, fatigue, nausea and vomiting. In young babies, parents might notice a bulging spot on their child’s head, a weak cry or unusual behavior.
Some red flags that are more specific to meningitis are a bruise-like purple rash, a stiff neck, confusion and sensitivity to light; these more neurological symptoms warrant immediate medical attention, said Kirsten Wiens, an infectious-disease epidemiologist and assistant professor at Temple University’s Barnett College of Public Health.
Prompt treatment is essential for a full recovery
If providers suspect meningitis, they’ll probably do a spinal tap to collect a sample of the fluid surrounding the spinal cord. This can reveal what specific pathogen is causing the infection, said Martinello, which helps medical providers determine the best treatment. If it is bacterial meningitis, you’ll be given antibiotics immediately.
“You have to really get the antibiotics going within minutes of [a patient] hitting the door, because that’s what’s going to save their lives,” said Beckham. “It’s a very rapidly progressive infection.” Things can get severe within a matter of hours, though most people can recover fully with quick treatment.
If you think you’ve been in contact with someone with meningitis, preventative antibiotics may also be recommended to reduce your chances of getting sick. “You would just go to your health care provider and say you’ve been exposed to someone who has meningococcal disease and they’ll prescribe you a course of antibiotics,” said Wallace.
Certain people are more susceptible to infection
Anyone can develop bacterial meningitis, but “the very young and very old,” tend to be more vulnerable, Boulware said, as well as those with weakened immune systems. The bacteria also transmit more easily in settings where many people live or gather, including in college dormitories, military barracks or nightclubs, such as the one linked to the recent outbreak in Kent.
“When you go to an army barracks or go to college in a dorm, you’re exposed to a bunch of new people, so they have different strains [of bacteria] you haven’t been exposed to,” Boulware said. This, combined with crowding and situations in which people might be kissing or sharing drinks can create ideal conditions for meningococcal bacteria to spread.
Different age groups are more likely to develop meningitis from certain types of bacteria. For example, newborns are most at risk from group B streptococcus, which is usually harmless in adults but can cause serious illness in young children. Adolescents, such as those living in college dorms, are more likely to be exposed to meningococcus, the N. meningitidis bacteria, as well as pneumococcus and Haemophilus influenzae.
Vaccination is the best way to stay protected
General healthy habits, such as staying home if you’re sick, avoiding others who may be sick and not sharing drinks or smoking can help prevent meningococcal disease and meningitis. But because the infection can be so dangerous when it does occur, and symptoms like a headache and fatigue are easy to dismiss, “the biggest risk is not being vaccinated,” said Martinello.
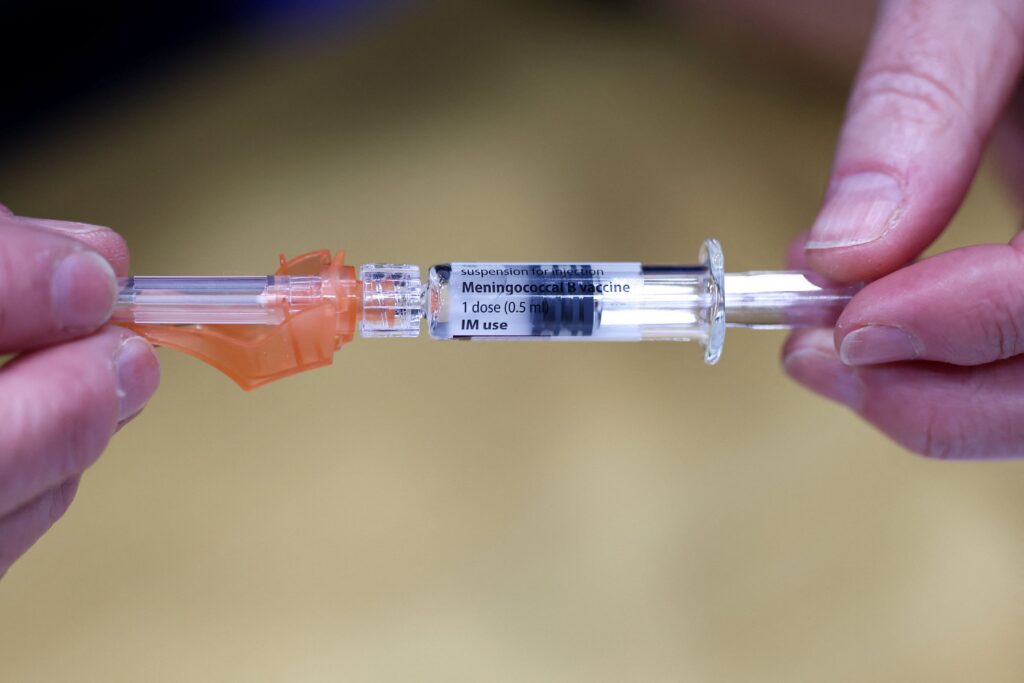
In the U.S., there are six vaccines available to protect against the most common variants of meningococcal disease. With these vaccines, protection wanes over time, so they are recommended at 11 to 12 years old (for the MenACWY vaccine), 16 years old (for a MenACWY booster) and between ages 16 and 18 for the MenB vaccine.
“The highest peak and highest risk of carrying the organism in your airway is in that late-adolescence, early-adulthood time frame,” said Beckham, “so the vaccines are all targeted to that age group for that very specific reason.”
Although the Centers for Disease Control and Prevention recommends meningococcal vaccination for all preteens and teens, children between ages 2 months and 10 years who are at increased risk, and adults at increased risk, these recommendations may change: In January, the CDC updated its childhood immunization schedule to mark some vaccines, including MenB, as “shared clinical decision-making,” meaning they would no longer be universally recommended for adolescents.
A number of medical groups led by the American Academy of Pediatrics filed a legal motion to contest these policy changes. Last week, a judge temporarily blocked the Trump administration from implementing these changes while the case proceeds.
Some experts fear that should this recommendation change go through, many adolescents would miss out on protection from meningitis when they’re most vulnerable. “I’m not really happy about it,” said Wallace. “The disease can be deadly, and the vaccine is safe and effective.”
The post 5 things you need to know about meningitis appeared first on Washington Post.