On March 6, Japan’s Ministry of Health, Labor and Welfare officially granted conditional and time-limited marketing authorization to two regenerative medical products derived from reprogrammed iPS cells, marking exactly 20 years since the creation of mouse iPS cells. These will be the world’s first practical application of iPS cell-derived products.
“We are very pleased to have taken a major step toward social application on the 20th anniversary of the announcement of mouse iPS cells,” said Shinya Yamanaka, director emeritus of the iPS Cell Research Institute at Kyoto University. “To establish it as a medical treatment, it is essential to go through the process of confirming its safety and efficacy in many more cases. I believe it is important that we continue to move forward steadily, step by step, with scientific caution and without getting carried away.”
What Are iPS cells?
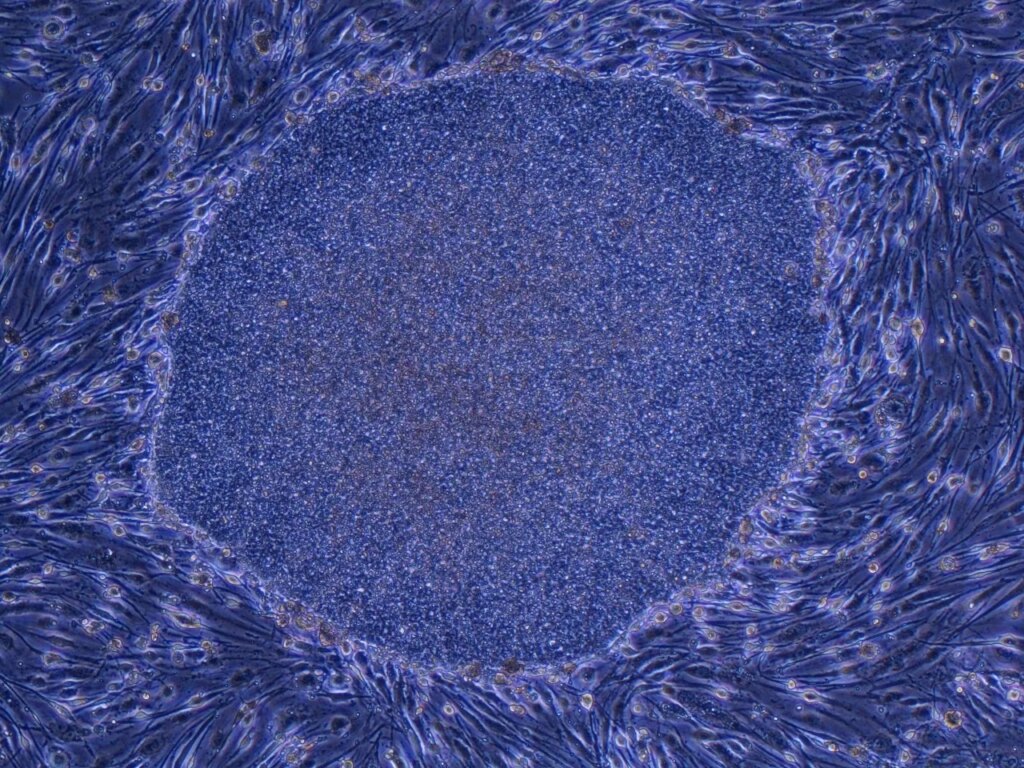
The initialism stands for induced pluripotent stem cells. These are adult cells, such as skin or blood cells, that have been reprogrammed to function like embryonic stem cells. They can divide indefinitely and can take the form of any cell type. Thanks to this ability, they can be used to test new drugs and for research in regenerative medicine. This type of cell allows for scientific advancement without the ethical problems that arise from working with embryonic stem cells.
Sheets of Cells Attached to the Wall of the Heart
One of the regenerative medicine products that has been approved is ReHeart, from Qualipse, a startup based at Osaka University. It’s a sheet of specialized heart cells called cardiomyocytes differentiated from iPS cells of healthy donors, and it generated considerable buzz when it was presented at the Osaka-Kansai Expo. It’s intended for patients with severe heart failure due to ischemic cardiomyopathy who don’t recover sufficiently despite standard treatment, including drug therapy and invasive procedures.
Severe heart failure is a serious condition that worsens over time, and the only treatment options are a heart transplant or a heart-assisted artificial heart. However, heart transplantation is hampered by a shortage of donors and age restrictions, and artificial hearts also carry the risk of infection and cranial nerve damage, as well as long-term decline in quality of life.
ReHeart addresses these unmet medical needs. The transplant is performed via a surgery in the left side of the chest, with three sheets of cardiomyocytes attached to the surface of the heart. Signaling proteins secreted by the transplanted cells help increase blood flow and repair tissue. In a national multicenter collaborative study that included eight patients with severe heart failure, a trend toward improvement was confirmed in four patients, with peak oxygen consumption (VO2 peak) increasing by more than 10 percent at 52 weeks post-transplant.
Neurons “Implanted” Directly Into the Brain
The second approved product is Amusepri (generic name: laguneprocell) from Sumitomo Pharma and Racthera. It consists of precursor cells destined to become dopamine-producing neurons made from donor iPS cells. It is indicated for improving motor symptoms in patients with Parkinson’s disease who have had an inadequate response to existing drug therapies, including levodopa-containing preparations.
Parkinson’s disease is a neurodegenerative disorder that causes motor symptoms such as tremors in the limbs and muscle rigidity due to the gradual loss of dopaminergic nerve cells in the brain. Current drug therapies are treatments to alleviate symptoms, not a fundamental approach to replacing lost nerve cells.
AmShepli aims to offer a new treatment option by transplanting progenitor cells from lost dopamine-making neurons directly into the brain. This transplant is performed using a minimally invasive type of brain surgery. Small holes are drilled in the skull, one on each side, and the cells are dispersed and injected into the capsule on both sides via three delivery routes.
In a physician-led trial conducted at Kyoto University Hospital, four of the six Parkinson’s disease patients analyzed showed an improvement in their off-time score (the score when the drug’s effect has worn off) on the Motor Symptoms Diagnostic and Treatment Rating Scale (MDS-UPDRS Part III) 24 months after transplantation. Researchers confirmed that the cells remained viable in all six patients at the transplant site.
World’s First Manufacturing Facility and Industry-Academia Collaboration
SMaRT, located in Suita City, Osaka Prefecture, is responsible for the production of Amshepri and is the world’s first commercial manufacturing facility dedicated to regenerative medicine and cell-based drugs derived from donor iPS cells. The iPS cells used as raw material for the product come from a stock provided by the Kyoto University iPS Cell Research Foundation, and the differentiation induction and manufacturing technologies are based on proprietary technologies from Kyoto University and other institutions. For example, Eisai’s cell purification technology is used in part of the manufacturing process; the product was made possible through collaboration between industry and academia, with contributions from various institutions.
It could also be argued that the fact that this groundbreaking approval came from Japan was structurally inevitable. This is because the entire supply chain has been almost entirely completed in Japan, from the establishment of the basic technology by Shinya Yamanaka, winner of the 2012 Nobel Prize in Physiology or Medicine, to the supply of iPS cells by the Kyoto University iPS Cell Research Foundation, the differentiation induction and manufacturing technologies developed by Kyoto University and other institutions, the establishment of the commercial manufacturing facility SMaRT, and even the development of university startups and the entry of major pharmaceutical companies.
The two new products are considered “approved with conditions and timeframes. ”This means that, even after approval, the products’ efficacy and safety must continue to be verified through post-marketing clinical trials and end-use studies.
This unique Japanese system has enabled early approval in fields such as regenerative medicine, where large-scale clinical trials are difficult to conduct, and is one of the factors explaining the practical application of these products. Furthermore, the approval process, including long-term public funding from national institutions, was not only the result of individual researchers but also the product of Japanese science policy.
A comprehensive study of ReHeart’s use outcomes in a target number of 75 patients is planned, with sales starting around the fall of 2026. AmShepli is also required to gather data for official approval.
This Is the Beginning of Regenerative Medicine
Transplantation of any of these products is not a treatment available to everyone at this stage and will be available as an insured treatment once the insurance coverage procedure—where the product is officially registered as covered by public health insurance—has been completed. The estimated timeframe for these products to be included on the insurance list is three months after approval for pharmaceuticals and four to five months after application for medical supplies, so it is still expected to be some time before they reach patients.
Commenting on the approval, Kenichiro Ueno, minister of health, labor, and welfare, stated at a press conference: “I am very pleased that a therapeutic product from Japan based on professor Yamanaka’s iPS cells has been put into practice for the first time in the world, and I hope it will help patients not only in Japan but all over the world.”
Jun Takahashi, director of the iPS Cell Research Institute at Kyoto University, who led the Amusepuri trial, stated: “The results of the deliberations are a major step forward, but even if approval is granted, that is not the goal, but only the beginning of this new medicine.” He emphasized the importance of accumulating long-term data, starting carefully with a limited number of cases.
Twenty years have passed since the emergence of iPS cells. The technology, which originated in the laboratory, has reached the stage where human cells are cultured, differentiated, and finally administered to the patient’s body. The future of medicine, rewritten by iPS cells, has only just begun.
This story originally appeared in WIRED Japan and has been translated from Japanese.
The post Japan Approves the World’s First Treatment Made With Reprogrammed Human Cells appeared first on Wired.