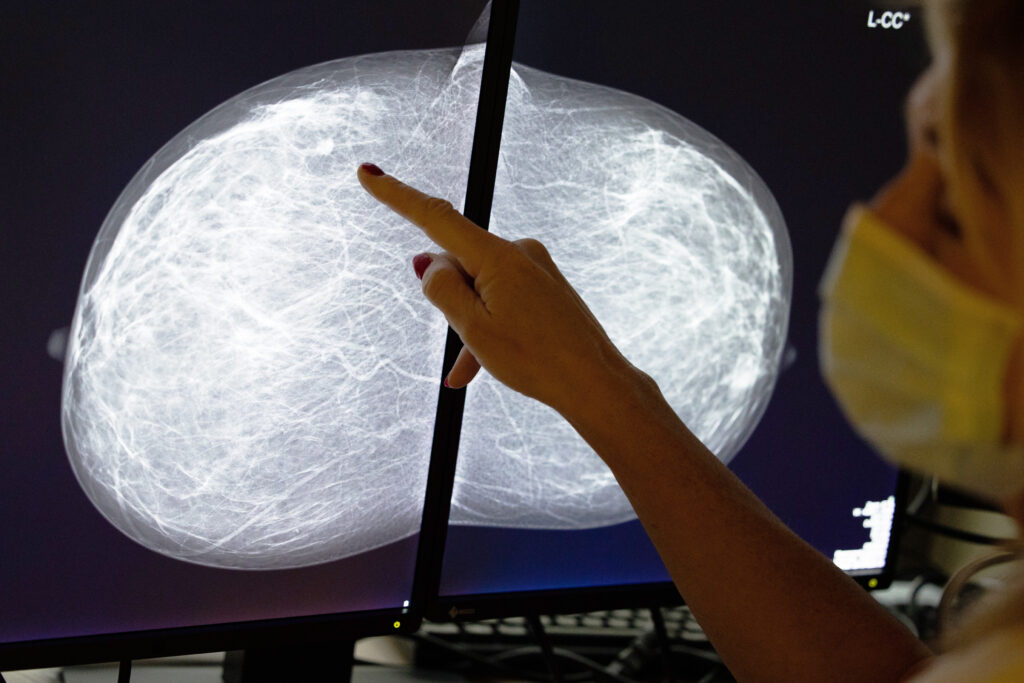
Routine mammograms that screen for breast cancer can also flag the risk of heart disease, the leading and often underrecognized cause of death in women, according to a new study in the European Heart Journal.
For decades, radiologists have observed that breast cancer screening scans also reveal calcium deposits in the arteries woven through breast tissue, which cause the blood vessels to stiffen.
The new study shows how artificial intelligence can be used, at scale, to opportunistically turn this “incidental finding” into a warning system for an entirely different category of disease. Researchers used AI to quantify the calcium deposits on arteries in more than 120,000 breast cancer screening scans and found that more severe breast artery calcification (BAC) was a marker of increased risk for heart failure, heart attacks, stroke and death.
The public health opportunity to flag hidden risks for heart disease is potentially massive: more than 40 million people get mammograms in the U.S. each year. Studies have shown that many women mistakenly believe that breast cancer is the leading cause of death, and they may not take as seriously the much greater risk of heart disease.
“If there is a way to educate women in a place ‘where they are’ anyway, like when getting a mammogram, it could be a game changer,” said Mary Cushman, a professor of pathology and laboratory medicine at the Larner College of Medicine at the University of Vermont. Cushman, who was not involved in the study, added that one of the most interesting findings was that the method could predict risk in women younger than 50.
“It is a clarion call that younger women do have risk, that it can be detected, and that detection of risk should lead to interventions to reduce risk, even at young ages,” Cushman wrote in an email.
She added that this does not mean a cancer screening should replace traditional monitoring of cardiovascular risk.
A hidden killer
For years, evidence has accumulated that heart disease in women is being missed — despite a large body of knowledge about how to prevent it. A recent report from the American Heart Association showed that cardiovascular disease is increasing sharply in women, even as awareness of the risk among women is declining. By 2050, a third of women between the ages of 20 and 44 will have some form of heart disease. High blood pressure, obesity and diabetes are all projected to increase.
“Women are very under-screened and under-detected for cardiovascular disease,” said Hari Trivedi, associate professor of radiology at Emory University and a leader of the study.
That led Trivedi and colleagues to wonder if a different kind of screening could provide an opportunity to catch people who could be slipping through the cracks — nearly 70 percent of women who are 40 or older are up to date on their mammograms, according to an American Cancer Society report.
The study population included 74,000 women who received mammograms at Emory Healthcare in Atlanta and nearly 50,000 from Mayo Clinic Enterprise, based in Arizona, Florida, the Midwest and Rochester, Minnesota. In the Emory patient population, only about 7 percent of people had enough data in their medical records to calculate a standard cardiovascular risk score, and in the Mayo population about 28 percent did.
Trivedi and colleagues devised an AI algorithm to quantify the level of calcium deposits in their breast cancer scans and categorized them into four broad categories along a continuum, from zero evidence of calcified arteries to severe. Then, they saw how predictive those categories were of major cardiovascular events in the women, who had been followed for a median of seven years.
They found that the BAC score was a powerful way to flag risk. Between two women who looked similar across other attributes, such as age, race and known cardiovascular risk factors, those in the “severe” category had double the risk of having a cardiovascular event of someone with no calcification, the study found.
Trivedi said that clinical trials are planned to begin later this year to further validate the approach. In the future, researchers hope that this information could help lead to new therapies or interventions.
AI algorithms already on offer
There is already AI software from the company CureMetrix that has been cleared by regulators to detect calcification in mammograms. Some clinics already offer this add-on service to women, sometimes for an additional out-of-pocket cost. Doctors were hesitant to give medical advice, but pointed out that the main value of the test right now would be to flag women who were ignoring their heart health and not seeing a primary care doctor for traditional cardiovascular screening, such as monitoring blood pressure and cholesterol.
“I love the technology and I love the test, but the answer is there is not yet any evidence to support that having a BAC score can alter your care or management,” Trivedi said.
Several physicians who are enthusiastic about the potential for this kind of screening to improve women’s health warned that its true power will come from being applied as a screening tool on all scans as a public health benefit and not just as an add-on service available only to people who have the means and interest to pay extra.
Lori B. Daniels, director of the cardiovascular intensive care unit at the University of California at San Diego who was not involved in the study, wrote an accompanying editorial calling to report this measure consistently.
“If radiologists start reporting it, we’ll start to accumulate the data we need — that’s the first step,” Daniels said. “There’s a trove of data here that’s been ignored.”
While scientists want to learn more about how this information can improve clinical care, she points out that doctors already know how to prevent heart disease. The scans also may be more compelling to patients than abstract cholesterol numbers from a lipid panel run on their blood.
“Sometimes when people see a visualization of what’s going on in their arteries, something clicks and they get motivated,” Daniels said.
correctionA previous version of this article incorrectly listed the state of a Mayo Clinic location. It is in Rochester, Minnesota, not Rochester, New York.
The post The surprising way breast cancer screenings could reveal heart disease appeared first on Washington Post.